How to Lower Fasting Blood Sugar Naturally (Morning, Pregnancy, Prediabetes, Diabetes)

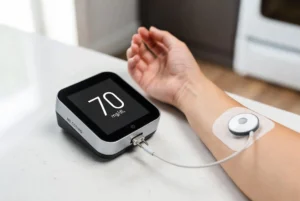
Have you ever woken up, checked your levels, and wondered, “Why is my fasting blood sugar high?” It is incredibly frustrating when you have been “good” all day. You might feel like your body is playing a trick on you.
Don’t worry, you are not alone in this morning mystery. Many patients I consult with through Federa deal with this exact issue. Learning how to lower fasting blood sugar naturally does not have to be a medical maze.
Whether you have prediabetes, type 2, or are pregnant, small shifts make a huge impact. In this guide, we will break down why those numbers creep up overnight.
We will also explore science-backed ways to wake up with better results. Let’s get your health back on track together.
Why Fasting Blood Sugar Is High in the Morning
Many people feel confused when their morning numbers are high. You haven’t eaten for eight hours, so why are the levels up? This usually happens because of your liver.
While you sleep, your liver releases glucose to give you energy. This is a normal process. However, insulin resistance can make this process go into overdrive. This is often called the “dawn phenomenon.”
During a recent clinical intake at Federa, a patient named Mark shared his struggle. He noticed his fasting blood sugar was high in the morning but normal all day. We discovered his liver was overcompensating.
According to the American Diabetes Association (ADA), hormones like cortisol also play a role. These hormones peak in the early morning. They tell your body to wake up and get moving.
Because of this, your blood sugar might rise before you even touch a bagel. This is especially true if your body cannot use insulin effectively. Understanding this “why” is the first step toward better health.
Healthy & Normal Fasting Blood Sugar Levels
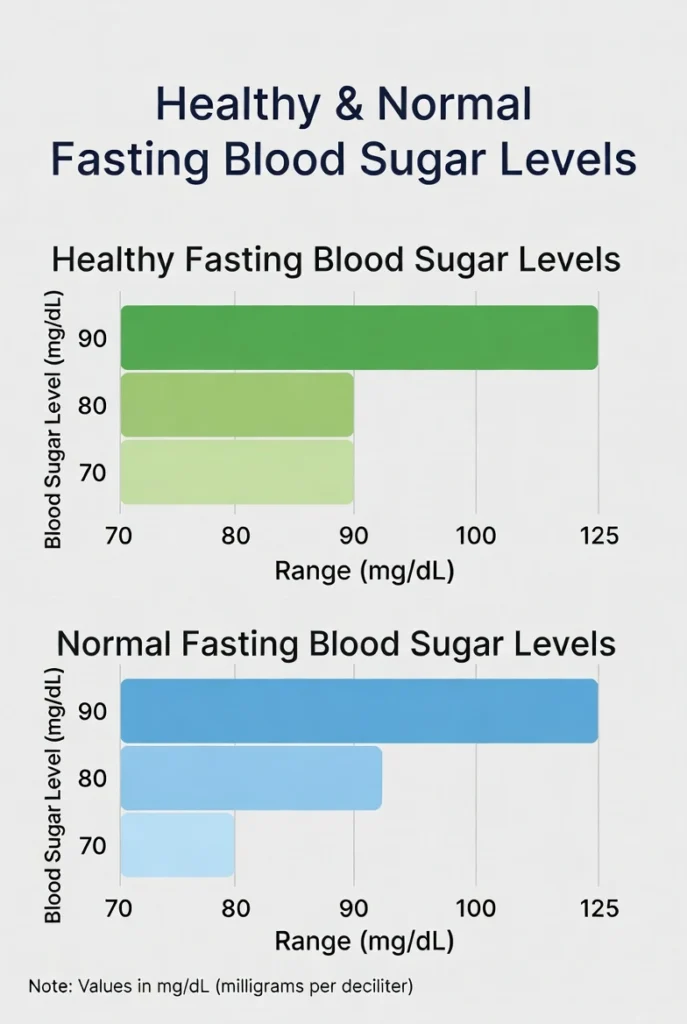
It is important to know what your target should be. “Normal” can look different based on your age and health status. Most doctors look at a window of 8 to 12 hours of fasting.
| Condition | Normal Fasting Range (mg/dL) | When to Take Action |
| Healthy Adult | 70–99 | Monitor if consistently near 100 |
| Pregnancy | Under 95 | Consult OB if over 95 |
| Prediabetes | 100–125 | Focus on lifestyle changes |
| Diabetes | 126+ | Work with a clinical team |
Are you seeing a fasting blood sugar over 100? If so, it is time to look at your evening habits. A level of 110 or 120 indicates your body needs some support.
Similarly, a fasting blood sugar of 140 in the morning suggests significant insulin resistance. You should always discuss these numbers with your primary care physician. They can help rule out other underlying issues.
What Can Throw Off a Fasting Glucose Test?
Sometimes, a high reading is just a fluke. Several factors can mess with your results. First of all, think about your sleep. Did you toss and turn all night?
Poor sleep increases cortisol, which spikes glucose. Furthermore, a late-night snack can linger in your system. If you ate a heavy carb meal at 11 PM, your 7 AM test will be high.
Dehydration is another common culprit. When you are low on water, your blood becomes more concentrated. This makes your glucose levels look higher than they actually are.
Also, consider your stress levels. Are you worried about the test itself? Interestingly, even a minor cold or infection can raise your morning numbers. Your body releases sugar to fight the illness.
Finally, ensure you check your blood sugar at the right time. The best time to check blood sugar in the morning is immediately after waking. Waiting too long can allow the dawn phenomenon to intensify.
Dawn Phenomenon & Insulin Resistance Explained
The dawn phenomenon is a natural surge in blood sugar. It happens to everyone, even people without diabetes. However, those with insulin resistance feel the effects much more.
Between 4:00 AM and 8:00 AM, your body releases growth hormones. These hormones temporarily decrease your insulin sensitivity. As a result, your blood sugar levels begin to climb.
In a healthy body, insulin steps in to keep things level. But if you have insulin resistance, your cells ignore the insulin. Consequently, the sugar stays in your bloodstream instead of fueling your cells.
High stress also makes this worse. Cortisol is a “stress hormone” that triggers glucose release. If you are chronically stressed, your morning spikes will likely be more dramatic.
To stop the dawn phenomenon naturally, you must improve insulin sensitivity. This involves a mix of movement, diet, and stress management. We will cover those specific strategies in the next sections.
How to Lower Fasting Blood Sugar Naturally
Focusing on lifestyle is the most effective way to see permanent change. You cannot just look at what you eat. You must look at how you live your entire day.
First, prioritize your sleep schedule. Aim for 7 to 9 hours of quality rest. Studies show that even one night of bad sleep increases insulin resistance. This leads to higher morning numbers.
Second, manage your evening light exposure. Blue light from phones can disrupt your circadian rhythm. When your internal clock is off, your metabolism suffers. Try to put the phone away an hour before bed.
Third, find a way to de-stress. Whether it is deep breathing or a short walk, lower your cortisol. Because lower cortisol means less glucose released by your liver overnight.
Finally, consistency is more important than restriction. Do not try to change everything in one day. Instead, pick one habit to master this week. This approach leads to long-term success.
How to Lower Fasting Blood Sugar in the Morning

If you wake up high, you want answers fast. While there is no “30 second morning glucose flush” that works miracles, you can take action. Start your day with a large glass of water.
Hydration helps your kidneys flush out excess sugar. After that, get your body moving. A 10-minute brisk walk can help your muscles soak up that extra glucose.
You do not need a high-intensity workout. In fact, gentle movement is often better for morning spikes. It lowers sugar without causing a secondary stress response.
Also, consider your breakfast choices. Many people think they should skip breakfast to lower sugar. However, this can sometimes make the liver release more sugar.
Instead, eat a high-protein breakfast. Think eggs or Greek yogurt. This tells your liver that you have plenty of energy. As a result, it may stop pumping out extra glucose.
Best Diet Strategies to Lower Fasting Blood Sugar
Your evening meal is the biggest predictor of your morning glucose. This is where most people make mistakes. To fix this, we need to focus on “protein-first” dining.
During my research at Federa, we found that carb-heavy dinners are the main culprits. If you eat pasta late at night, your sugar will stay elevated for hours. Instead, try a low-carb diet for your final meal.
Focus on fiber-rich vegetables and lean proteins. For example, salmon with broccoli is an excellent choice. The fiber slows down digestion, preventing a massive overnight spike.
Another great strategy is carb timing. If you want carbs, eat them earlier in the day. Your body is generally more insulin-sensitive in the afternoon than in the late evening.
What about intermittent fasting? Some find it helpful, but be careful. Extreme fasting can sometimes trigger the liver to release sugar. It is better to have a consistent 12-hour fasting window.
For instance, eat dinner at 7 PM and breakfast at 7 AM. This gives your body enough time to process food without feeling “starved.” This balance is key for steady levels.
What to Eat (and Drink) at Night to Lower Fasting Blood Sugar
Many people think they must stop eating entirely after 6:00 PM. However, the right bedtime snack can actually stabilize your morning numbers. This is especially true if you experience the “Somogyi effect,” where sugar drops too low at night, causing a rebound spike.
So, what should you eat at night to lower fasting blood sugar? The best approach is a combination of protein and healthy fats. For instance, a small handful of walnuts or a tablespoon of peanut butter on celery works wonders. These slow-digesting foods provide a steady energy source.
Furthermore, consider magnesium-rich foods like pumpkin seeds. Magnesium plays a vital role in glucose metabolism. Similarly, a small bowl of low-fat cottage cheese is an excellent choice. It contains casein protein, which digests slowly over several hours.
When it comes to drinks, stay away from diet sodas or sugary teas before bed. Instead, try a cup of herbal chamomile tea. It helps lower stress and improves sleep quality. Some people also find success with a tablespoon of apple cider vinegar in a large glass of water.
In fact, research suggests that acetic acid in vinegar may improve insulin sensitivity overnight. Just be sure to rinse your mouth afterward to protect your tooth enamel. Avoiding late-night alcohol is also crucial, as it can interfere with the liver’s glucose regulation.
Exercise to Lower Fasting Blood Sugar
Physical activity is like a natural “vacuum” for blood sugar. Your muscles use glucose for energy even without needing extra insulin. This is why exercise is a cornerstone for anyone learning how to improve insulin sensitivity naturally.
The timing of your workout matters significantly. A post-dinner walk is one of the most effective blood sugar management tips. Even a 15-minute stroll around the block can significantly lower the glucose peak after your final meal.
Additionally, resistance training is incredibly beneficial. Building lean muscle mass allows your body to store glucose more efficiently as glycogen. Therefore, try to include two or three days of weight lifting or bodyweight exercises each week.
Don’t forget about morning light movement. If you wake up with a high reading, don’t panic. Instead, do some light stretching or a few air squats. This helps signal to your body that the “fast” is over and it’s time to use the sugar in your blood.
Consistency is the secret sauce here. You don’t need to run a marathon to see results. Rather, focus on being active throughout the day. Frequent, short bursts of movement are often better than one long session at the gym.
Supplements & Natural Remedies (Evidence-Based)
While no pill can replace a healthy diet, certain supplements may help support your goals. It is important to remember that these are not “cures.” However, they can provide an extra edge when used correctly alongside lifestyle changes.
Magnesium for fasting blood sugar control is one of the most well-studied options. Many people with insulin resistance are actually deficient in this mineral. Taking a high-quality magnesium glycinate supplement at night may improve both sleep and glucose levels.
Fiber supplements, such as psyllium husk, are also helpful. Taking fiber before your largest meal slows down sugar absorption. This prevents the massive spikes that lead to high fasting numbers the next day.
You may have heard of berberine or cinnamon. Some studies show berberine can be as effective as some common medications for glucose control. However, it can cause stomach upset in some people. Always consult a healthcare professional before starting new natural remedies for high fasting blood sugar.
Vitamins like Vitamin D also play a role. Low levels of Vitamin D are often linked to higher risks of prediabetes. Ensuring your levels are optimal supports overall metabolic health. Again, use these as “tools” in your kit, not as a total solution.
How to Lower Fasting Blood Sugar Without Medication
If you are looking to fix high fasting blood sugar without a prescription, you must focus on your “metabolic flexibility.” This means teaching your body how to switch between burning sugar and burning fat efficiently.
Start by reducing your overall glycemic load. This doesn’t mean “zero carbs,” but rather choosing complex carbs over simple sugars. For instance, swap white rice for quinoa or cauliflower rice. This simple change reduces the burden on your pancreas.
Another tip is to stay hydrated throughout the night. Keep a glass of water on your nightstand. If you wake up, take a few sips. This helps keep your blood volume stable and prevents glucose concentration.
Managing your stress is also non-negotiable. Chronic stress keeps your “fight or flight” system active, which pumps sugar into your blood. Try 5 minutes of box breathing before you sleep. It sounds simple, but it effectively lowers cortisol.
Finally, be patient with your body. If you are wondering how to prevent high fasting blood sugar, know that it takes time for your liver to adjust. Your body is a complex system, and it prefers gradual changes over radical shifts.
How to Lower Fasting Blood Sugar During Pregnancy
Managing glucose during pregnancy requires an extra level of care. If you are dealing with gestational diabetes, your fasting number is often the hardest to control. It is important to stay calm—stress only makes the numbers go higher.
I recently spoke with a patient who was frustrated because she followed her meal plan perfectly, yet her morning numbers stayed high. We found that she was going too long without eating. For many pregnant women, a late-night protein snack is essential.
Try eating a snack right before bed that includes protein and a complex carb. An example would be an apple with almond butter or a slice of whole-grain toast with a hard-boiled egg. This prevents the liver from “dumping” sugar in the middle of the night.
Safe movement is also key. A gentle 10-minute walk after dinner is usually OB-approved and very effective. It helps your body process the evening meal before you lay down for the night.
Always work closely with your maternal-fetal medicine specialist or dietitian. They may suggest specific timing for your checks. Remember, these strategies are meant to support you and your baby’s health safely.
How Long Does It Take to Lower Fasting Blood Sugar?
Everyone wants to know how long to lower fasting blood sugar. Typically, you might see small changes in 3 to 7 days of consistent habit tracking. However, significant changes in your A1C and fasting baseline usually take 2 to 3 months.
How many days of fasting to lower blood sugar depends on your level of insulin resistance. Don’t get discouraged if the scale or the glucose monitor doesn’t move immediately. Your cells need time to “repair” and become sensitive to insulin again.
FAQ Section
How can I lower my fasting blood sugar in the morning? The fastest way is to hydrate with water and engage in 10-15 minutes of light exercise, like walking. This helps your muscles burn off the excess glucose released by your liver overnight.
Why is my fasting blood sugar high but my A1C is normal? This often happens due to the “dawn phenomenon” or poor sleep. Your A1C is a 3-month average, so it can hide short morning spikes if your levels are perfect the rest of the day.
Is 105 blood sugar after eating normal? Yes, a reading of 105 mg/dL one to two hours after a meal is generally considered excellent and within the healthy range for most people.
Can stress cause a 130 fasting blood sugar? Absolutely. High stress triggers cortisol, which signals the liver to release glucose. If you had a very stressful night or poor sleep, your fasting number could easily jump into the 130s.
Will drinking water at night lower my morning sugar? While water doesn’t “dissolve” sugar, staying hydrated prevents your blood from becoming concentrated. This can prevent “false” high readings caused by dehydration.
Conclusion
Learning how to lower fasting blood sugar naturally is a journey of consistency. There are no overnight miracles, but there are daily victories.
By focusing on protein-rich dinners, better sleep, and gentle movement, you can take control of your health. Remember, your morning number is just one data point—it doesn’t define your success. Always consult with your healthcare provider before making major changes to your routine.
References
- American Diabetes Association (ADA) / StatPearls: Dawn Phenomenon: Pathophysiology and Management
- National Institutes of Health (NIH) / PMC: Magnesium and Type 2 Diabetes: A Review
- Centers for Disease Control and Prevention (CDC): Monitoring Your Blood Sugar
- Mayo Clinic: Gestational Diabetes: Diagnosis and Treatment
- Harvard Health Publishing / NIH: Physical Activity/Exercise and Diabetes Position Statement