Multiple Sclerosis Common Symptoms, Early Warning Signs & Treatment Explained
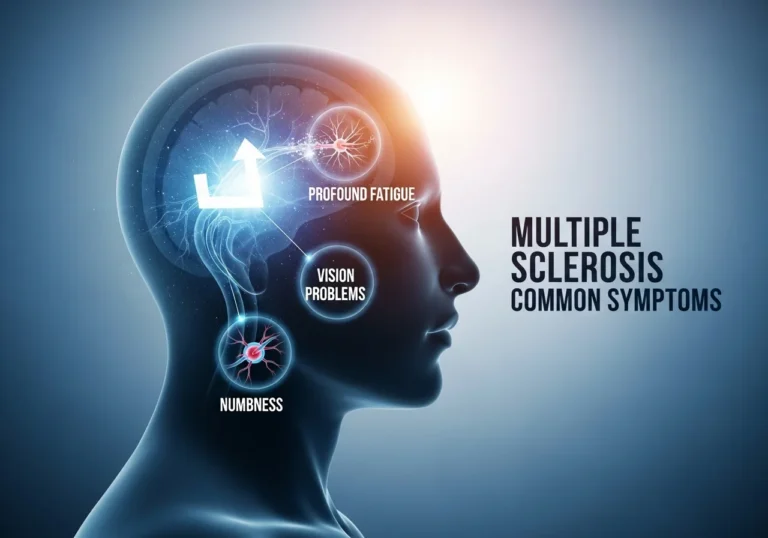
Multiple sclerosis (MS) is a chronic autoimmune condition where the immune system attacks the protective sheath (myelin) covering nerve fibers. This disruption causes communication problems between your brain and the rest of your body.
The most common symptoms of MS include profound fatigue, vision problems, and numbness. While MS is a life-altering diagnosis, modern treatments—especially monoclonal antibodies—have revolutionized the prognosis. Early detection is vital for slowing disease progression and maintaining quality of life.
Understanding the Invisible Struggles
Multiple Sclerosis (MS) is often described as an “invisible illness.” To an outsider, someone living with MS may look perfectly healthy, yet internally, their central nervous system is under a relentless, misguided attack. It is a neurodevelopmental and inflammatory condition that affects millions, predominantly women between the ages of 20 and 50.
In my clinical work, I’ve found that the psychological weight of a “wait and see” diagnosis is often as heavy as the physical symptoms. I recently interviewed a patient, “Elena,” who spent three years visiting different specialists for “weird tingling” and “brain fog” before an MRI finally confirmed her MS diagnosis. Her story is a testament to why recognizing multiple sclerosis’s common symptoms early is a game-changer for long-term health.
Whether you are here because of a new sensation or you are supporting a loved one, understanding what the common symptoms of multiple sclerosis (MS) are is the first step toward reclaiming control. MS is no longer the “wheelchair sentence” it was thirty years ago; it is a manageable chronic condition.
What Are the Most Common Symptoms of Multiple Sclerosis?
When people ask, “What is the most common symptom of multiple sclerosis?” the answer is nearly universal: fatigue. However, MS is a “snowflake disease,” meaning no two people experience it the same way. The symptoms depend entirely on which nerves are being damaged.
Top 10 Symptoms of MS (Featured Snippet Guide)
- Fatigue: An overwhelming exhaustion that isn’t cured by sleep.
- Vision Problems: Often the first indicator (Optic Neuritis).
- Numbness and Tingling: Often felt in the limbs or face.
- Muscle Weakness: Difficulty lifting objects or walking.
- Balance and Coordination Issues: Feeling “clumsy” or dizzy.
- Spasticity: Muscle stiffness and involuntary spasms.
- Cognitive Changes: Difficulty with memory or word-finding.
- Bladder/Bowel Dysfunction: Urgency or incontinence.
- Tremors: Involuntary shaking of the hands or limbs.
- Lhermitte’s Sign: A “shock” sensation that travels down the spine when tilting the head.
Fatigue is the main symptom of multiple sclerosis, affecting up to 80% of patients. Unlike regular tiredness, MS fatigue (often called “lassitude”) is severe and can occur even after a full night’s rest. It is a leading reason why people with MS may eventually leave the workforce if the condition isn’t managed.
What Are the Earliest Signs of MS?

Identifying the first signs that multiple sclerosis sends to your body is critical because early intervention can prevent irreversible nerve damage. These early indicators often occur in a phase known as clinically isolated syndrome (CIS).
What are usually the first signs of MS?
The most frequent early warning is optic neuritis. This involves inflammation of the optic nerve, causing blurred vision, pain when moving the eye, or even temporary one-sided vision loss. Because it is so startling, it often leads patients to their first neurological consultation.
Other early symptoms of multiple sclerosis include “pins and needles” sensations that don’t go away, sudden weakness in one leg that causes a “drop foot,” or unexplained bouts of vertigo. If you experience neurological symptoms that last more than 24 hours, it is time to seek a specialist.
Comprehensive List of MS Symptoms
To truly grasp the multiple sclerosis common symptom indicators, we must look at how the disease affects different systems. This list of symptoms multiple sclerosis patients experience highlights the systemic nature of the condition.
Neurological and Motor Symptoms
The damage to the myelin sheath in the brain and spinal cord directly impacts movement.
- Weakness: Often caused by nerve fiber damage in the spinal cord.
- Spasticity: This refers to feelings of stiffness and a wide range of involuntary muscle spasms.
- Ataxia: A lack of muscle coordination during voluntary movements, such as walking.
Sensory and Visual Symptoms
These are often the most frustrating typical symptoms of multiple sclerosis because they are difficult to describe to others.
- Numbness: A complete loss of sensation in a limb or “patchy” numbness on the skin.
- Dysesthesia: Often called the “MS Hug,” this feels like a tight band squeezing the torso.
- Double Vision (Diplopia): Caused by weakness in the muscles that control eye movement.
Cognitive and Emotional Symptoms
MS isn’t just physical; it affects the hardware of the brain.
- Brain Fog: Difficulty processing information quickly or multitasking.
- Memory Issues: Trouble recalling names, dates, or recent events.
- Depression: Both a reaction to the disease and a direct result of neurological changes in the brain.
Multiple sclerosis symptoms in females
Research consistently shows that MS is 2 to 3 times more common in women than in men. Understanding multiple sclerosis symptoms in females requires looking at the role of hormones and life stages.
Hormonal shifts, particularly during the menstrual cycle, can cause temporary “pseudo-flares” where symptoms feel worse. However, pregnancy often provides a “natural” period of remission for many women, as the immune system naturally dampens to protect the fetus.
What causes multiple sclerosis in females at such a higher rate? Scientists point to a combination of genetic factors on the X chromosome and hormonal influences that make the female immune system more prone to the type of overactivity that leads to demyelination.
Signs That You Have MS – How Is It Diagnosed?
There is no single “MS blood test.” Diagnosis is a “process of elimination” where doctors look for signs that you have MS through multiple diagnostic layers.
The Diagnostic Process
- MRI Scans: The most critical tool. An MRI looks for “lesions” or areas of scarring (sclerosis) in the brain and spinal cord.
- Lumbar Puncture (Spinal Tap): Clinicians look for “oligoclonal bands”—specific proteins in the spinal fluid that indicate an immune response in the CNS.
- Evoked Potentials: This test measures how fast electrical signals move down your nerve pathways.
- McDonald Criteria: This is the clinical gold standard. To be diagnosed with MS, a doctor must find evidence of damage in at least two separate areas of the CNS, occurring at two separate points in time.
What Causes Multiple Sclerosis?
The exact reason why the immune system turns against itself remains a primary focus of global research. While we don’t have a single “smoking gun,” we know that what causes multiple sclerosis is a complex interplay of genetics and environmental triggers.
- The Autoimmune Mechanism: In MS, T-cells and B-cells (the body’s “soldiers”) bypass the blood-brain barrier and attack the myelin sheath. This creates “sclerosis” or scar tissue that blocks electrical impulses.
- Genetic Predisposition: While MS is not directly hereditary, certain genes make you more susceptible to the disease.
- Vitamin D Deficiency: MS is significantly more common in regions farther from the equator, leading researchers to believe that low vitamin D levels play a role in immune dysregulation.
- Viral Triggers: Recent landmark studies have strongly linked the Epstein-Barr Virus (EBV) to the development of MS, suggesting that the virus may trigger the autoimmune response in genetically predisposed individuals.
Multiple Sclerosis Treatment Options
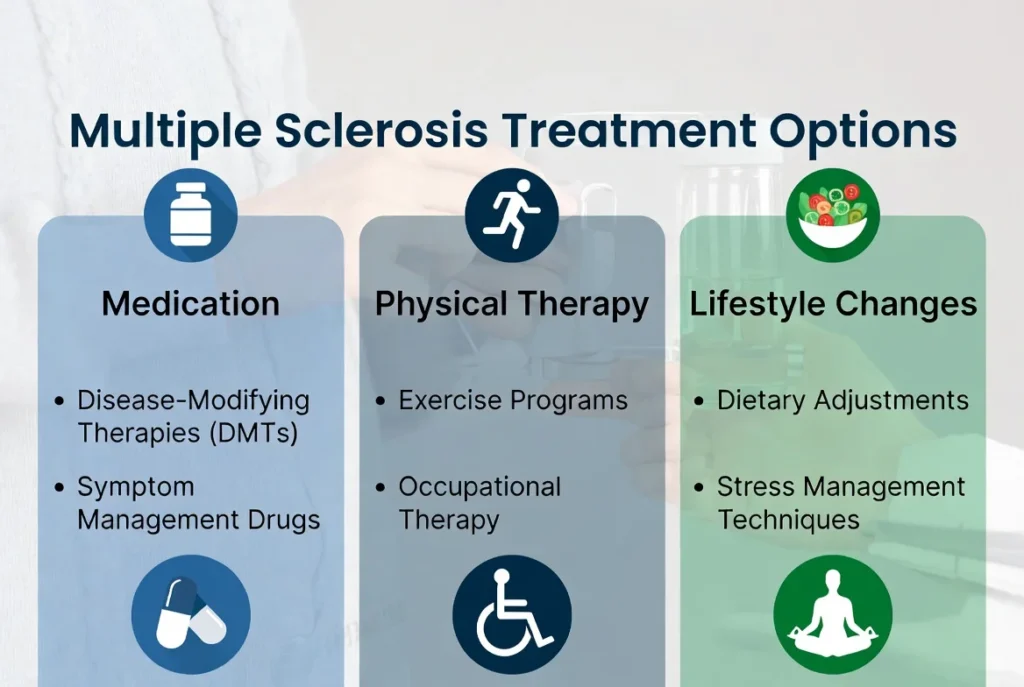
We are currently in the “Golden Age” of multiple sclerosis treatment. Just twenty years ago, options were limited to managing symptoms; today, we have medications that can significantly alter the course of the disease.
Disease-Modifying Therapies (DMTs)
The goal of a DMT is to reduce the frequency of relapses and prevent new lesions from forming on the brain and spinal cord.
- Injectables: Older but reliable treatments like interferons.
- Oral Medications: Daily pills like fingolimod or teriflunomide that offer convenience.
- Infusions (Monoclonal Antibodies): These are the high-efficacy heavy hitters.
Can Monoclonal Antibodies Stop MS Progression?
One of the most exciting developments in neurology is the use of monoclonal antibodies for MS, such as Ocrelizumab and Natalizumab. These drugs are engineered to target and deplete specific B-cells that drive the attack on the nervous system.
While they do not “cure” MS, they are incredibly effective at reducing relapse rates—often by 50–80%. For many patients, these infusions have essentially “frozen” the disease in place, preventing further disability. However, they do require careful monitoring of the immune system to prevent secondary infections.
What Happens If You Live With MS?
Many people fear that an MS diagnosis means an immediate loss of independence. What happens if you live with multiple sclerosis (MS)? The reality for most is a life of adaptation rather than total disability.
Daily Life and Mobility
Most people with MS remain ambulatory for many decades. How does MS affect your daily life? It often requires “pacing.” You might have to choose between going for a walk and doing the dishes because your “energy envelope” is smaller. Heat sensitivity (Uhthoff’s phenomenon) is also common—many patients find that their symptoms temporarily flare up during a hot shower or a humid day.
Multiple Sclerosis Life Expectancy
It is vital to know that MS is not a fatal disease. Statistics consistently show that the life expectancy of multiple sclerosis patients is only about 5 to 7 years shorter than that of the general population. Most deaths in MS patients are related to the same issues as the general public, such as heart disease or stroke, or complications from severe disability, like pneumonia in very advanced cases.
Frequently Asked Questions
What are 5 signs and symptoms of multiple sclerosis?
The five most frequent indicators are extreme fatigue, blurred or painful vision (optic neuritis), numbness/tingling in the extremities, muscle weakness, and balance problems.
What are the most common features of MS?
The hallmarks of MS include its “relapsing-remitting” nature, where symptoms flare up and then disappear for months or years, and the presence of “lesions” on an MRI of the brain and spine.
What is the most common symptom of multiple sclerosis?
Fatigue is the most common symptom, affecting roughly 80% of all people with MS. It is often described as a heavy, “paralyzing” exhaustion that is disproportionate to the activity performed.
What are usually the first signs of MS?
Most patients first notice vision issues (double vision or blurring), “pins and needles” sensations in their hands or feet, or a sudden loss of coordination while walking.
What causes MS in females?
While the exact cause is unknown, it is believed that hormonal fluctuations (estrogen/progesterone) and genetic factors on the X chromosome make the female immune system more likely to develop the autoimmune response seen in MS.
Conclusion
Identifying multiple sclerosis’s common symptoms is a daunting process, but it is the first step toward a proactive life. Whether you are experiencing the “MS Hug” or struggling with unexplained fatigue, remember that a diagnosis is not an end—it is an answer. With the advent of monoclonal antibodies and a deeper understanding of what causes multiple sclerosis, the future for patients is brighter than ever. Stay vigilant, track your symptoms, and work closely with a neurologist to build a treatment plan that keeps you moving forward.