Jaw Pain for Heart Attack: Symptoms, Location, and Warning Signs Explained

In my years practicing emergency medicine, I have seen countless patients walk into the ER rubbing their face, convinced they just need a dentist. However, jaw pain for heart attack is a critical, often misunderstood warning sign that can mean the difference between life and death.
Just last month, I treated a 62-year-old patient named Sarah who complained of a strange, dull ache in her lower jaw that simply would not subside. She had no chest pain, yet a routine EKG revealed she was in the middle of a severe myocardial infarction.
While not all jaw discomfort equates to a cardiac event, recognizing a jaw pain heart attack warning is absolutely vital. Many cases of facial aching are indeed simple dental issues or temporomandibular joint (TMJ) disorders.
However, when jaw pain acts as a referred pain symptom of myocardial ischemia, ignoring it can be fatal. This is especially true for higher-risk groups, including women, diabetics, and older adults, who frequently present with these atypical symptoms.
In this comprehensive guide, we will explore the anatomy of cardiac jaw pain, symptom patterns, how to differentiate it from TMJ, and the critical jaw pain heart warning signs that require immediate emergency care.
Key Takeaways
- Jaw pain can be a critical, referred symptom of a heart attack, caused by shared nerve pathways between the heart and the face.
- Cardiac jaw pain typically feels like a dull, heavy pressure in the lower jaw, not a sharp, localized toothache.
- Women and diabetics are far more likely to experience jaw pain as their primary heart attack symptom, often without any classic chest pain.
- If your jaw ache worsens with physical exertion or is accompanied by shortness of breath, nausea, or chest pressure, it is a medical emergency.
- Never attempt to self-diagnose severe facial pain that arises suddenly; always err on the side of caution and consult a physician.
What Is Jaw Pain for Heart Attack?
To understand cardiac jaw pain, we must look at how the human nervous system is wired. When the heart muscle experiences a lack of oxygen-rich blood—a condition known as myocardial ischemia—it sends panic signals to the brain.
However, the heart does not have a high density of distinct pain nerve endings as your skin does. Instead, the heart shares a central nerve pathway with several other areas of the upper body.
This shared neurological highway primarily involves the vagus nerve and the trigeminal nerve pathways. When the brain receives distress signals from the struggling heart muscle, it often gets “confused” about the origin of the pain.
Because the brain is more accustomed to processing sensory input from the jaw, neck, and arms than from the heart itself, it projects the sensation of pain onto those areas. This medical phenomenon is known as referred pain.
Therefore, jaw discomfort and heart issues are deeply connected through your neurological wiring. During a cardiac event, a patient might experience classic chest pressure, but they are just as likely to feel intense aching in their jaw, neck, or shoulders.
It is crucial to understand that jaw pain and chest pain are incredibly common in the ER. The pain is usually not sharp; rather, cardiac jaw pain is frequently described as a dull, radiating pressure that feels like a heavy weight pressing against the bones of the face.
Location of Jaw Pain During a Heart Attack
A frequent question I hear from concerned patients is, “Where is jaw pain for heart attack usually felt?” Pinpointing the exact jaw pain heart attack location can help differentiate a cardiac emergency from a routine dental issue.
Most commonly, the discomfort targets the lower jaw, medically known as the mandible. Patients rarely describe pain in the upper jaw or cheekbones when suffering from a heart attack.
Left-Sided vs Bilateral Pain
When asking where you get jaw pain for a heart attack, the left side is the most frequently reported location. This aligns with the classic left-arm radiation that many associate with cardiac events.
However, it is a dangerous myth to assume it only happens on the left. Where would jaw pain be for heart attack if the ischemia is widespread? It can easily present on the right side, or even as bilateral pain, affecting both sides of the lower jaw simultaneously.
Radiation to the Neck and Ears
Cardiac jaw pain rarely stays in one tiny, isolated spot. It is a diffuse discomfort that tends to travel.
The pain often radiates upward from the chest, moving through the throat and neck before settling into the lower jawbone. In some severe cases, patients report that the heavy, aching sensation extends all the way back to the earlobes.
Sensations Associated with Cardiac Jaw Pain
Understanding the exact characteristics of the pain is just as important as knowing its location. If you are wondering what jaw pain feels like for a heart attack, you must think in terms of pressure rather than a sharp, localized injury.
Dull Pressure and Heaviness
What type of jaw pain for a heart attack should you look out for? Unlike a toothache, which is usually a sharp, stabbing, and highly localized pain, cardiac jaw pain is broad.
Patients often describe it as an intense tightness, a dull ache, or a severe heaviness, as if their jaw is being clamped or squeezed. Some individuals even mistake it for a severe sinus headache or the onset of a stress-induced tension headache.
Consistency and Exertion Triggers
Another critical factor is the timing. Is heart attack jaw pain constant? The answer is no; it frequently fluctuates.
The pain may come and go over several hours or even days leading up to the main cardiac event. A massive red flag is if the jaw pain worsens with physical exertion or emotional stress and completely subsides when you sit down and rest.
This exertion-triggered aching is a classic sign of angina—a warning that your heart is struggling to pump enough blood through narrowed arteries. If your jaw hurts when you walk up a flight of stairs but stops when you sit, you need an immediate cardiac evaluation.
Heart Attack Warning Signs With Jaw Pain
Jaw pain rarely occurs in total isolation during a major cardiac event. It is usually accompanied by a cascade of other physiological warning signs.
Recognizing a jaw pain heart attack warning requires looking at the entire clinical picture. If your jaw ache is paired with any of the following symptoms, treat it as a life-threatening emergency:
- Chest pressure or squeezing: A feeling like an elephant is sitting on your chest, which may radiate upward into the jaw pain chest pathway.
- Shortness of breath: Struggling to catch your breath, even while resting or doing minimal physical activity.
- Cold sweat: Suddenly breaking out in an unexplained, clammy, cold sweat.
- Severe fatigue or dizziness: Feeling lightheaded, unexpectedly exhausted, or on the verge of fainting.
- Nausea or vomiting: Severe stomach upset that mimics food poisoning, often accompanied by jaw and chest discomfort.
Jaw Pain Heart Attack Men vs Women
In cardiovascular medicine, we have learned the hard way that male and female hearts often sound the alarm quite differently. Understanding the nuances of a jaw pain heart attack man presentation versus a female presentation is critical for preventing misdiagnosis.
Historically, medical textbooks focused almost entirely on male heart attack symptoms. For men, a heart attack typically presents in the “classic” Hollywood fashion: crushing central chest pain that shoots down the left arm.
While men can certainly experience a jaw pain heart attack warning, it is usually accompanied by unmistakable chest pain.
Conversely, women are far more likely to experience “atypical” cardiac symptoms. A woman’s heart attack might manifest entirely as severe lower jaw pain, profound unexplained fatigue, indigestion, or pain between the shoulder blades.
Because women do not always experience the classic chest clutching, their symptoms are frequently dismissed as anxiety, acid reflux, or a simple TMJ flare-up. If you are a woman experiencing sudden, unexplained facial aching, you must advocate for yourself and request an immediate EKG.
Jaw Pain vs Other Conditions
As an ER doctor, my first job is to play detective. When a patient presents with facial discomfort, I must quickly differentiate between jaw pain, heart attack, TMJ disorder, or a localized dental infection.
Temporomandibular joint (TMJ) disorders affect the hinge joint connecting your jaw to your skull. TMJ pain is usually sharp, highly localized to the joint itself, and almost always triggered by the mechanical action of chewing or wide yawning. You will often hear a distinct popping or clicking sound when you move your mouth.
Dental issues, such as an abscessed tooth, also cause severe facial aching. However, a sore jaw heart attack presentation is vastly different from a toothache. Dental pain is usually isolated to a specific tooth or gum area and is intensely aggravated by hot or cold temperatures.
To help clarify, here is a differential diagnosis breakdown:
| Localized directly to the jaw joint (near the ear) | Pain Type | Location | Primary Trigger |
| Heart attack | Dull, pressure, heavy ache | Lower jaw, often radiates to chest/neck | Physical exertion, emotional stress |
| TMJ disorder | Sharp, aching, accompanied by clicking | Localized directly to the jaw joint (near ear) | Chewing, yawning, speaking |
| Dental issue | Sharp, throbbing, highly localized | Specific tooth or gum line | Biting down, hot/cold liquids |
When to Worry About Jaw Pain
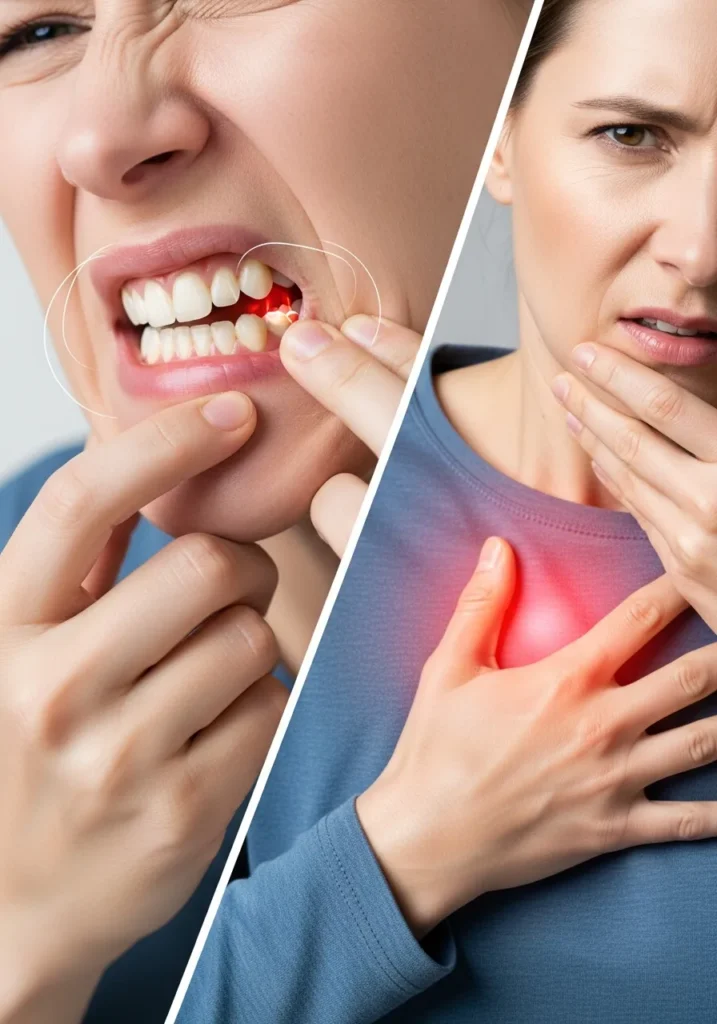
Not every facial ache requires an ambulance, but knowing exactly when to worry about jaw pain is your best defense against a catastrophic cardiac event. You must look for the “red flag” combinations.
If your jaw discomfort occurs entirely on its own and only hurts when you bite down on an apple, it is likely a dental issue. However, if the jaw pain chest connection becomes apparent—meaning you feel pressure in your jaw and your chest simultaneously—you are in the danger zone.
You should treat your jaw pain as a life-threatening medical emergency if it is accompanied by shortness of breath, a cold sweat, or sudden dizziness.
Furthermore, if the pain begins abruptly while you are exercising, shoveling snow, or walking upstairs, and it forces you to stop and rest, do not ignore it. Call emergency services immediately.
How Long Before a Heart Attack Does Jaw Pain Occur?
Patients frequently ask me, “How long do you have jaw pain before a heart attack actually happens?” Unfortunately, there is no standardized timeline for myocardial ischemia.
For some patients, the jaw ache hits like a lightning bolt just minutes before they collapse from a massive infarction. For others, the timeline is much more insidious.
I have heard many jaw pain heart attack stories where patients experienced a dull, throbbing lower jaw ache intermittently for weeks. This is a condition known as stable angina. The pain would flare up during their morning jog and disappear when they sat down.
This intermittent jaw discomfort is your heart’s early warning system. It is begging for more oxygen. If you catch this angina phase early and see a cardiologist, you can often prevent the actual heart attack from ever occurring.
Risk Groups & Clinical Context
Certain individuals must be hyper-vigilant regarding any unexplained jaw discomfort and heart issues. If you fall into a high-risk category, your threshold for seeking emergency care should be incredibly low.
Patients with a known history of coronary artery disease, high cholesterol, or hypertension already have compromised blood vessels. A sudden jaw ache in these individuals is highly suspicious for a cardiac event. Likewise, chronic smokers have heavily damaged arterial walls, drastically increasing their clot risk.
Diabetics require special mention. Long-term diabetes causes neuropathy (nerve damage) throughout the body, including the nerves surrounding the heart.
Diabetics are at a massive risk for “silent ischemia,” where they suffer a heart attack without feeling any chest pain at all. For a diabetic patient, a sudden jaw ache or bout of nausea might be the only warning sign they receive.
Frequently Asked Questions
How do I know if jaw pain is a heart attack?
You cannot definitively know without medical testing, but cardiac jaw pain is usually a dull, heavy pressure rather than a sharp pain. It is highly suspicious if it worsens with physical exertion, radiates down to your chest, or is accompanied by sweating and shortness of breath.
Is heart attack jaw pain on both sides?
Yes, it can be. While it is commonly reported on the left side of the lower jaw, cardiac referred pain can easily present on the right side or as bilateral pain affecting both sides of the face and neck simultaneously.
When to worry about jaw pain?
You should worry and seek immediate emergency care if the jaw pain is sudden, feels like a squeezing pressure, occurs during physical activity, or is paired with chest tightness, nausea, dizziness, or pain radiating down your arm.
What hurts first before a heart attack?
The initial pain varies wildly. Some people feel a sudden, crushing chest pressure first. Others may experience early warning signs days in advance, such as a dull ache in the lower jaw, unexplained back pain between the shoulder blades, or severe heartburn that antacids cannot fix.
What are the four signs your heart is quietly failing?
Signs of quiet heart failure include profound, unexplained fatigue during normal activities; chronic shortness of breath (especially when lying down flat); sudden fluid retention causing swelling in the legs or ankles; and a rapid, irregular heartbeat.
Conclusion
As an emergency medicine physician, the most tragic cases I see are the ones where a patient felt something was wrong but convinced themselves it was “nothing serious.” Jaw pain for a heart attack is one of the most deceptive warning signs your cardiovascular system can produce.
Because it does not always fit the classic Hollywood image of a man clutching his chest in agony, it is far too easy to brush off as stress, a dental issue, or a TMJ flare-up. However, your heart relies on shared nerve pathways to signal severe distress.
When your heart muscle is starving for oxygen, that ischemia often manifests as a heavy, dull ache in your lower jaw. This is especially true for women, older adults, and diabetics, who frequently experience these atypical symptoms instead of traditional chest pain.
Remember, it is always better to visit the emergency room for a false alarm than to ignore a myocardial infarction. If your jaw pain is accompanied by chest pressure, shortness of breath, a cold sweat, or if it worsens with physical exertion, do not wait to see a dentist. Call 911 immediately.
For more life-saving information and to understand other critical vascular events, I highly encourage you to read our comprehensive guide on Stroke vs Heart Attack or review our detailed breakdown of Heart Attack Symptoms. Knowledge and rapid action are your absolute best defenses against cardiovascular disease.