What Is Blood Sugar? Understanding Glucose in Your Body

Have you ever felt a sudden, exhausting crash in energy after a heavy lunch and wondered exactly what is blood sugar and how it dictates your daily life? You are certainly not alone in this curiosity, as many people struggle to understand their body’s internal fuel system.
As a physician, I frequently explain to my clinic patients that grasping the fundamentals of blood glucose is the absolute first step toward mastering your long-term metabolic health. In simple medical terms, blood sugar—clinically referred to as blood glucose—is the primary sugar circulating within your bloodstream.
It is derived directly from the carbohydrates and foods you eat, serving as your body’s main, essential source of daily energy. Your vascular system constantly carries this [glucose] to every single one of your body’s cells, from your brain to your muscles, providing the power they need to function properly.
However, much like a high-performance engine, your complex biological system requires precisely the right amount of fuel to run smoothly and efficiently. Maintaining a healthy, delicate balance is absolutely critical for your overall longevity.
If your blood glucose levels chronically stay too high (hyperglycemia) or suddenly dip dangerously low (hypoglycemia), it can quickly lead to severe, cascading health complications.
In this comprehensive medical guide, we will break down the exact science of blood sugar, explain how to accurately interpret your daily lab readings, and detail the actionable steps you can take right now to keep your numbers safely within the optimal target zone.
How Is Blood Sugar Measured? Understanding Tests and Units
In the medical field, we use specific standardized tests to determine how your body is handling glucose. In the United States, we measure glucose in milligrams per deciliter (mg/dL). If you are reading research from Europe or Canada, you might see millimoles per liter (mmol/L).
When a patient comes into my clinic, I don’t just look at one number. We use a variety of tests to get a complete “metabolic picture.” Understanding the types of blood sugar tests available helps you and your care team make informed decisions.
Standard Clinical Glucose Tests
The most common assessment is the Fasting Blood Sugar (FBS) test. This requires you to abstain from food for at least eight hours. It provides a baseline of how your body manages sugar without the influence of a recent meal.
Another vital tool is the HbA1c (A1c) test. Unlike a daily finger stick, the A1c measures your average blood sugar over the past two to three months. It essentially shows how much “sugar coating” is on your red blood cells.
| Test Type | Purpose | Timing |
| Fasting Glucose | Measures baseline sugar levels | After 8+ hours of fasting |
| HbA1c | 3-month average glucose | Any time (no fasting needed) |
| Postprandial | Checks the response to food | 2 hours after a meal |
| Oral Glucose Tolerance | Checks for gestational diabetes | Timed intervals after a sugar drink |
What is blood sugar called on a blood test? You will usually see it listed simply as “Glucose” or “GLU.” If you are looking at your long-term average, look for “Hemoglobin A1c.”
Normal Blood Sugar Levels and Healthy Ranges
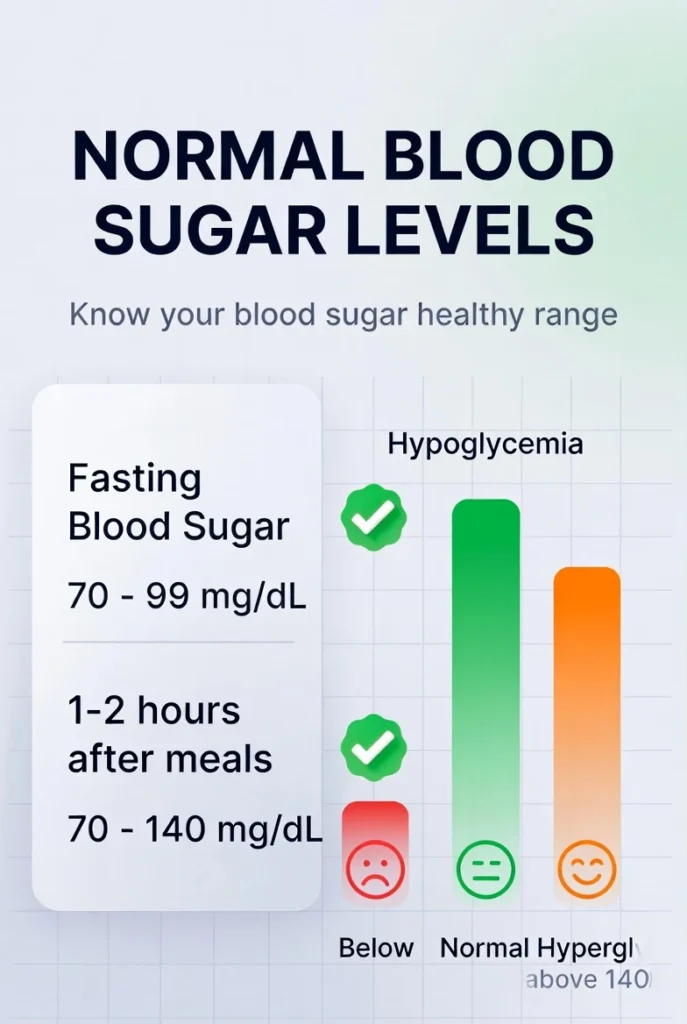
One of the most frequent questions I receive is, “What is a blood sugar level supposed to be?” While “normal” can vary slightly based on age and health status, the medical community generally agrees on specific ranges for healthy adults.
Healthy Fasting Ranges
For someone without diabetes, a normal fasting blood sugar level is typically between 70 and 99 mg/dL. If your fasting level is between 100 and 125 mg/dL, it often indicates prediabetes. This is a crucial “warning light” period where lifestyle changes can often reverse the trend.
Post-Meal Expectations
It is perfectly normal for your blood sugar to rise after you eat. However, a healthy body should bring those levels back down quickly. Ideally, two hours after a meal, your blood sugar should be less than 140 mg/dL.
| Category | Fasting Level (mg/dL) | 2 Hours After Meal (mg/dL) |
| Normal | 70–99 | Less than 140 |
| Prediabetes | 100–125 | 140–199 |
| Diabetes | 126 or higher | 200 or higher |
I remember a patient, Mark, who was confused by his blood sugar reading. He felt great, but his fasting glucose was 115 mg/dL. By explaining that he was in the “prediabetes” range, we were able to adjust his fiber intake and walking routine, bringing him back to a normal blood sugar level within six months.
Low Blood Sugar (Hypoglycemia) Explained
While we often focus on high sugar, low blood sugar (hypoglycemia) is equally important. In clinical terms, hypoglycemia occurs when your glucose drops below 70 mg/dL. This is often a side effect of diabetes medications, but it can also happen due to excessive exercise or skipping meals.
Recognizing the Signs
When your brain doesn’t get enough glucose, it sends out emergency signals. You might feel shaky, sweaty, dizzy, or suddenly irritable (often called being “hangry”). In severe cases, it can lead to confusion or even fainting.
Immediate Action Steps
If you feel these symptoms, we follow the “15-15 rule.” Eat 15 grams of fast-acting carbohydrates—such as 4 ounces of fruit juice or 5 pieces of hard candy—wait 15 minutes, and check your level again.
What to eat when blood sugar is low:
- Half a banana
- A tablespoon of honey
- Glucose tablets
- 4 ounces of regular (not diet) soda
What level of blood sugar is dangerous? Anything below 54 mg/dL is considered severely low and requires immediate medical attention. It is vital to carry a fast-acting carb source if you are prone to these dips.
High Blood Sugar (Hyperglycemia) Explained
On the other end of the spectrum is high blood sugar, known as “hyperglycemia.” This happens when your body has too little insulin or cannot use insulin effectively. Chronic high sugar is the hallmark of diabetes and can damage blood vessels over time.
Identifying Hyperglycemia Symptoms
High sugar often acts as a “silent” condition, but there are red flags. I ask my patients to look for the “Three Polys”: polyuria (frequent urination), polydipsia (excessive thirst), and polyphagia (excessive hunger).
What are 5 signs your blood sugar is too high?
- Blurred vision
- Unexplained fatigue
- Slow-healing sores or cuts
- Frequent headaches
- Dry mouth and itchy skin
When Is It an Emergency?
What is a dangerous level of blood sugar? If your blood sugar is consistently over 240 mg/dL, you may be at risk for a life-threatening condition called ketoacidosis. If you experience nausea, vomiting, or breath that smells fruity, seek emergency care immediately.
Understanding what to do when blood sugar is high is essential. For most, this involves staying hydrated with water, taking prescribed medications, and performing light activity like a 15-minute walk to help muscles burn off the excess glucose.
Blood Sugar Spikes and Regulation
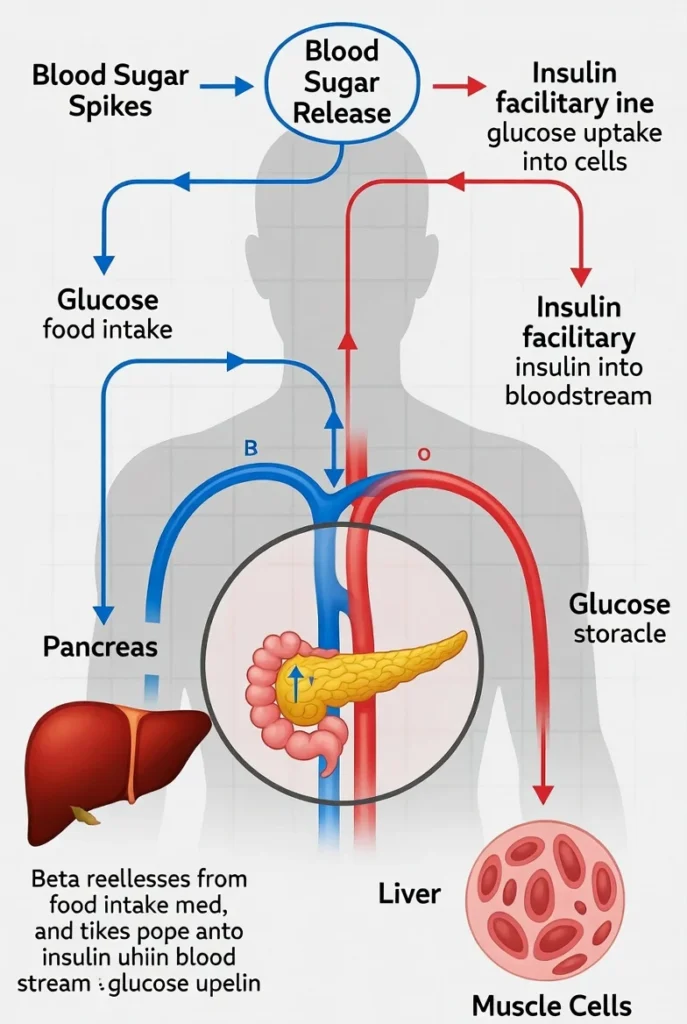
A blood sugar spike is a rapid increase in glucose levels shortly after eating. While spikes are common after eating refined carbs or sugary treats, frequent “rollercoaster” spikes can damage your arteries and increase your risk for heart disease.
The Science of Regulation
The primary driver of blood sugar regulation is the pancreas. This organ acts like a thermostat. When sugar rises, it releases insulin, a hormone that acts as a key to let glucose into your cells. When sugar drops, it releases glucagon, which tells your liver to release stored glucose.
Blood glucose explanation simplified: Think of insulin as the delivery driver and your cells as the customers. If the driver is on strike (type 1 diabetes) or the customers won’t open the door (type 2 diabetes/insulin resistance), the glucose just sits in the street (your bloodstream), causing a traffic jam.
Factors like stress can also cause spikes. When you are stressed, your body releases cortisol, which tells the liver to dump extra energy into the blood for a “fight or flight” response. This is why your blood sugar reading might be high even if you haven’t eaten a single carb.
Factors Affecting Blood Sugar
Many people assume that food is the only thing that moves the needle on their glucose meter. However, as I often explain during patient consultations, your blood sugar reading is a reflection of your entire lifestyle.
Many hidden variables can cause your levels to drift out of the normal blood sugar range.
Diet and the Glycemic Index
The most obvious factor is your carbohydrate intake. Simple carbs, like white bread and sugary drinks, cause a rapid blood sugar spike. On the other hand, complex carbs paired with fiber, protein, and healthy fats digest more slowly. This slower digestion leads to a more stable energy curve rather than a sharp peak.
Physical Activity
Exercise is one of the most powerful tools for blood sugar regulation. When you move your muscles, they can take up glucose from your blood even without the help of insulin. This is why a short walk after a meal is so effective at lowering a post-meal spike.
Stress and Sleep
If you aren’t sleeping well, your body produces more cortisol. This stress hormone makes your cells less sensitive to insulin, causing your levels to climb. I have seen many patients who eat a perfect diet but still have high fasting sugar simply because they only sleep five hours a night.
Illness and Medications
When you are sick, your body’s immune response triggers the release of extra glucose for energy. Additionally, certain medications—especially steroids like prednisone—can cause significant hyperglycemia. Always keep a log of these factors to discuss with your healthcare provider.
Blood Sugar Monitoring and Management
In modern medicine, we have incredible tools for blood sugar monitoring. Gone are the days of just guessing how you feel. Today, we use technology to see exactly how your body responds to your daily choices in real-time.
Monitoring Devices
- Glucometers: These are traditional finger-stick devices. They give you a “snapshot” of your sugar at that exact moment.
- Continuous Glucose Monitors (CGMs): These are small sensors worn on the arm or belly. They provide a “movie” of your glucose 24/7, showing trends while you sleep or exercise.
Understanding what blood sugar monitoring is for you depends on your goals. For a person with Type 1 diabetes, a CGM is often a lifesaver. For someone interested in general wellness, checking fasting levels with a glucometer a few times a week might be enough.
Interpreting Your Trends
Don’t panic over a single high reading. Instead, look for patterns. Is your sugar always high on Monday mornings after a stressful weekend? Is it always low after your Tuesday gym session? These trends are much more valuable for blood sugar control than any single number.
Blood Sugar Support and Lifestyle Tips
If you are looking for what blood sugar support is, the answer lies in consistency. Small, daily habits are more effective than drastic, short-term diets. Here is how I coach my patients to maintain a healthy glucose profile naturally.
Nutritional Guidance
Focus on “the plate method.” “Fill half your plate with non-starchy vegetables (broccoli, spinach, peppers), one-quarter with lean protein (chicken, fish, tofu), and one-quarter with a high-fiber starch (quinoa, sweet potato). This balance prevents the dreaded blood sugar spike.
Supportive Nutrients
While not a replacement for medication, some supplements show promise in supporting healthy glucose metabolism.
- Magnesium: Helps with insulin sensitivity.
- Chromium: May assist in carbohydrate metabolism.
- Cinnamon: Some studies suggest it can slightly lower fasting glucose.
- Fiber: Essential for slowing sugar absorption.
Blood Sugar and Diabetes
It is a common misconception to ask, “Are blood sugar and diabetes the same?” In reality, blood sugar is a biological metric, whereas diabetes is a chronic condition where those metrics remain consistently high.
The A1c Correlation
If your average blood sugar reading is around 140 mg/dL, your A1c will likely be approximately 6.5%. This is the threshold where we officially diagnose Type 2 diabetes. Lowering your daily average by just 30 mg/dL can significantly reduce your risk of complications like kidney disease or nerve damage.
Practical Management
Managing diabetes is about staying in the “time in range.” This means keeping your levels between 70 and 180 mg/dL for as much of the day as possible. The more time you spend in this zone, the better you will feel and the lower your long-term risks will be.
Frequently Asked Questions
What is considered low blood sugar?
Low blood sugar, medically known as hypoglycemia, is clinically defined as any glucose reading dropping below 70 mg/dL. When you reach this dangerous level, you must immediately follow the standard 15-15 rule. This involves consuming exactly 15 grams of fast-acting carbohydrates, such as juice, and rechecking your blood sugar levels after 15 minutes to ensure stability.
What is considered high blood sugar?
For a fasting individual, any glucose reading measuring over 126 mg/dL is clinically considered high and may indicate diabetes. Alternatively, if you test your blood two hours after consuming a meal, any reading exceeding 180 to 200 mg/dL is officially classified as hyperglycemia. Consistently seeing these elevated numbers requires a comprehensive medical evaluation from your doctor.
What is a good blood sugar level?
An optimal, healthy fasting blood sugar level for most adults without diabetes falls perfectly between 70 and 99 mg/dL. However, for individuals actively managing diagnosed diabetes, their physician will typically set a slightly adjusted target range, aiming for readings strictly between 80 and 130 mg/dL before meals to maintain safe and stable metabolic balance.
What level of blood sugar is dangerous?
Any blood sugar reading soaring over 240 mg/dL is considered highly dangerous and requires immediate caution, as it can quickly trigger diabetic ketoacidosis. Conversely, a severe drop measuring below 54 mg/dL is equally life-threatening. This extreme low can rapidly cause sudden loss of consciousness and severe seizures and necessitates urgent emergency medical intervention to stabilize.
Can stress raise my blood sugar?
Yes, experiencing high emotional or physical stress absolutely spikes your blood sugar. Stress actively triggers the sudden release of survival hormones, including cortisol and adrenaline. These powerful hormones directly command your liver to dump extra stored glucose into your bloodstream, which can cause a very significant metabolic spike even if you have not recently eaten anything.
Conclusion
Understanding what blood sugar is is more than just memorizing a few numbers on a lab report. It is about recognizing how your body transforms food into the energy that powers your life. As we have explored, glucose is a vital fuel, but maintaining it within a normal blood sugar range requires a mindful balance of nutrition, movement, and stress management.
In my years of clinical practice, I have seen that patients who actively monitor their blood sugar readings are much better equipped to avoid the pitfalls of chronic hyperglycemia. Whether you are managing a diagnosis of diabetes or simply looking to optimize your daily energy levels, small adjustments can yield significant results.
Choosing whole foods over processed sugars and incorporating a simple evening walk can do wonders for your blood sugar regulation.
Remember, your health journey is personal. While this guide provides the scientific foundation for understanding glucose, it is not a substitute for professional medical care. If you notice persistent symptoms of high or low sugar, or if your blood sugar test results are outside the typical range, reach out to your doctor.
By staying informed and proactive, you can ensure that your blood sugar remains a source of vitality rather than a source of concern.