Blood Pressure During a Heart Attack: What’s Normal, High, or Low?
Experiencing severe chest discomfort is a terrifying event that prompts many people to immediately reach for their home blood pressure monitor. Patients frequently ask me what the exact blood pressure during a heart attack should look like, hoping for a definitive answer.
They assume that if their cardiovascular system is failing, their vital signs will clearly reflect that massive internal crisis.However, the medical reality is far more complicated and nuanced than most people realize.
Your numbers can fluctuate wildly depending on a variety of physiological factors, making home monitors unreliable for diagnosis. Relying solely on these numbers can provide a false sense of security or trigger unnecessary panic.
As a cardiologist, I constantly remind patients that there is no single magical reading that confirms or denies a cardiac event. This comprehensive medical guide will explain exactly how your vital signs react during a coronary crisis and why you must look beyond the numbers.
TL;DR: Quick Overview
- Highly Variable: Blood pressure can spike, drop, or remain completely normal during a heart attack.
- Not a Diagnostic Tool: There is no specific “heart attack blood pressure” number.
- Normal is Possible: Perfect blood pressure readings do not rule out a severe cardiac event.
- Diagnosis: Emergency doctors rely on ECGs, blood tests (troponin), and physical symptoms—never just home blood pressure readings.
What Is Blood Pressure During a Heart Attack?
Many people search for exactly what blood pressure is during heart attack events, expecting a specific numerical range. During a myocardial infarction, a coronary artery becomes blocked, starving a section of the heart muscle of oxygen.
This blockage initiates a massive, system-wide stress response that drastically alters your cardiovascular dynamics. Your body immediately recognizes that a vital organ is in distress and attempts to compensate.
The resulting blood pressure reading is essentially a tug-of-war between your nervous system’s panic response and your heart’s failing mechanical ability. Consequently, what the blood pressure is during heart attack events is highly unpredictable and unique to every single patient.
Normal vs High vs Low Blood Pressure During a Heart Attack
Understanding the differences between normal, high, and low readings during an event is crucial for grasping cardiovascular physiology. Each state tells a different story about how the body is handling the acute medical crisis.
High blood pressure during heart attack events is incredibly common in the early stages of the event. When intense chest pain strikes, your body releases a massive flood of adrenaline and cortisol into your bloodstream.
These stress hormones cause your blood vessels to constrict tightly, which naturally drives your blood pressure upward. Furthermore, patients with a history of chronic hypertension will likely continue to show elevated numbers during the emergency.
Experiencing normal blood pressure during heart attack emergencies is also a very frequent clinical presentation. If the blockage is relatively small or your heart is otherwise strong, your body might temporarily maintain perfect equilibrium.
The undamaged portions of your heart muscle simply work slightly harder to maintain adequate circulation. This is why having “perfect” vital signs at home should never stop you from calling an ambulance if you have chest pain.
Conversely, low blood pressure during heart attack scenarios is a severe and highly dangerous medical red flag. This typically occurs when a massive portion of the heart muscle dies, severely weakening the organ’s pumping ability.
The heart can no longer push blood effectively through your vascular system, causing your numbers to plummet rapidly. This state, known as cardiogenic shock, requires immediate, aggressive, and life-saving medical intervention in the emergency room.
Why Blood Pressure Varies During a Heart Attack
Patients constantly wonder how blood pressure during heart attack events is so wildly unpredictable across different individuals. The primary mechanism driving this variation is the autonomic nervous system, specifically the sympathetic and parasympathetic branches.
The sympathetic nervous system triggers the “fight or flight” response, heavily constricting arteries and raising your numbers. However, certain types of heart attacks, particularly those affecting the inferior wall of the heart, can stimulate the vagus nerve.
This parasympathetic stimulation does the exact opposite, aggressively slowing the heart rate and dropping blood pressure. Additionally, if a patient takes daily medications like beta-blockers or ACE inhibitors, their vital signs may be artificially suppressed despite the ongoing emergency.
Heart Rate and Blood Pressure During a Heart Attack
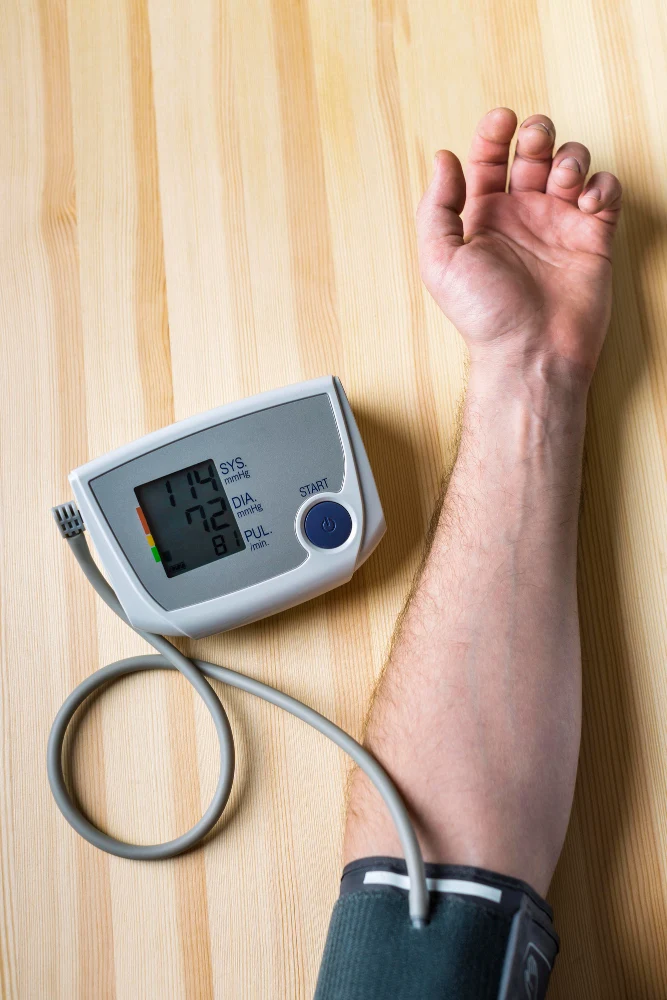
Analyzing the heart rate and blood pressure during heart attack emergencies provides a slightly clearer clinical picture. These two vital signs are deeply interconnected, though they may not always move in the same direction.
Your pulse and blood pressure during heart attack events usually respond initially to the intense surge of adrenaline. You will typically experience tachycardia, which is a very fast, pounding, and sometimes irregular heart rate.
However, if the electrical pathways of the heart are damaged by the lack of oxygen, the pulse may become dangerously slow. A weak, slow pulse combined with falling blood pressure indicates severe cardiovascular collapse.
Blood Pressure During a Heart Attack in Women
The clinical presentation of blood pressure during women’s heart attack events often differs from traditional male symptoms. Women frequently experience atypical physical signs, which can severely complicate the self-diagnosis process at home.
A female’s heart attack blood pressure reading might remain completely stable even while significant cardiac damage is occurring. Instead of classic chest pressure, women often present with profound fatigue, severe nausea, and a feeling of heavy indigestion.
Because their vital signs might appear perfectly fine, many women tragically delay seeking emergency medical help. It is absolutely critical for women to recognize these subtle warning signs regardless of what their home monitor displays.
Blood Pressure During a Heart Attack in Men
When examining blood pressure during heart attack scenarios, the signs usually align more closely with textbook descriptions. Men are statistically more likely to experience the classic, crushing “elephant on the chest” pain.
This intense, focused pain often triggers a highly aggressive sympathetic nervous system response. As a result, men frequently present in the emergency room with significantly elevated blood pressure and a rapid pulse.
They also more commonly report the classic symptom of pain radiating down the left arm and up into the jawline.
Can You Have a Heart Attack With Normal Blood Pressure and Pulse?
A very common and dangerous question is, “Can you have a heart attack with normal blood pressure and pulse?” The medical answer is an absolute and definitive yes.
Your heart is a remarkably resilient organ that can compensate for localized damage by overworking the healthy tissue. This compensatory mechanism can keep your vital signs looking beautifully normal for several hours.
Therefore, perfectly normal readings on your home machine absolutely do not rule out a life-threatening coronary blockage.
Does Blood Pressure Rise During a Heart Attack?
Many patients ask, “Does blood pressure rise during heart attack emergencies as a hard and fast rule?” While it frequently does, asking, “Do you have high blood pressure?” during heart attack events requires context.
In the early, acute phase of the event, the intense pain and panic almost always drive the numbers upward. The body is fighting the internal crisis by clamping down on blood vessels.
However, as the hours pass and the heart muscle becomes increasingly exhausted and damaged, the numbers will inevitably begin to fall.
Heart Rate During Heart Attack (Pulse Changes Explained)
Monitoring your heart rate during heart attack scenarios can reveal significant electrical disturbances within the organ. The pulse during heart attack emergencies is often the first vital sign to become erratic and unpredictable.
As the heart muscle is deprived of oxygen, the specialized cells that control your heartbeat begin to misfire. This can lead to dangerous arrhythmias, where the heart beats too fast to effectively pump blood.
Alternatively, if the blockage affects the specific artery supplying the natural pacemaker, the heart rate can drop to dangerously slow levels.
Borderline Heart Attack Blood Pressure — What It Means
People frequently search for a specific borderline heart attack blood pressure that acts as a warning threshold. Clinically, no such specific number or universal threshold exists in cardiology.
A reading of 140/90 might be a patient’s normal baseline, or it could represent a massive spike for someone usually at 110/70. Doctors do not diagnose myocardial infarctions based on a borderline reading.
Instead, we look for dynamic, ongoing changes in the electrocardiogram and highly specific cardiac proteins in your blood.
Can High Blood Pressure Cause a Heart Attack?
Understanding the long-term risks is vital, prompting the question can high blood pressure cause a heart attack eventually. Chronic, unmanaged hypertension is actually one of the leading root causes of coronary artery disease.
Over many years, the excessive physical force of high blood pressure damages the delicate inner lining of your arteries. This microscopic damage creates perfect catch-points for cholesterol to accumulate and form hard plaques.
Eventually, these hardened plaques can suddenly rupture, forming the exact blood clots that trigger a massive cardiac emergency.
Blood Pressure for Heart Attack Diagnosis
When considering the use of blood pressure for heart attack diagnosis, you must understand its limitations. Emergency medical personnel measure it immediately, but it is purely used as supporting clinical data.
It tells the physician how well your body is tolerating the ongoing physical stress. It dictates which specific emergency medications are safe to administer in the moment. However, it is never the primary tool used to definitively diagnose a blocked coronary artery.
Can a Heart Attack Last for Days?
Many patients are surprised when they ask can a heart attack last for days and hear the answer. While the acute, massive event is usually sudden, the underlying process can “stutter” over a long period.
Patients often experience a condition called unstable angina, where an artery partially blocks and unblocks repeatedly. This causes intermittent, severe chest pain that comes and goes over the course of several days or a week.
If this stuttering pain is ignored, it almost always culminates in a complete, permanent, and devastating arterial blockage.
Heart Attack Symptoms
Because vital signs are unreliable, you must focus heavily on recognizing the true physical heart attack symptoms. The most critical symptom remains a deep, heavy, squeezing pressure in the center of the chest.
This severe discomfort often radiates outward, affecting the shoulders, left arm, back, neck, or lower jaw. You may also experience a sudden, terrifying onset of shortness of breath without any physical exertion. Profuse, cold sweating, unexplained extreme dizziness, and a feeling of impending doom are also massive clinical red flags.
Blood Pressure During Heart Attack: Reddit Myths vs Facts
When patients experience anxiety, they often seek blood pressure during heart attack Reddit threads for rapid comfort. Unfortunately, anonymous internet forums are filled with incredibly dangerous medical misinformation and self-diagnosis guides.
Many online users falsely claim that if your top number is under 150, you are perfectly safe from a cardiac event. Others incorrectly state that taking an aspirin will immediately normalize your vital signs during an emergency.
You must completely ignore online diagnostic rules and rely strictly on professional medical evaluation in an emergency room.
When to Seek Emergency Help

Knowing exactly when to bypass your home monitor and call for professional help is crucial for survival. You must call emergency medical services immediately if you experience heavy chest discomfort lasting more than ten minutes.
If your chest pain is accompanied by severe shortness of breath or sudden, profound weakness, do not wait. Never attempt to drive yourself to the local hospital under any circumstances.
Calling an ambulance ensures that life-saving medical treatment and monitoring begin the moment paramedics arrive at your door.
Frequently Asked Questions
What is the most typical blood pressure during a heart attack?
There is absolutely no typical reading during a cardiac event. It varies drastically based on the patient’s baseline health, pain levels, and the severity of the heart muscle damage.
Can you have a heart attack if your blood pressure is 120/80?
Yes, you can have absolutely perfect, textbook vital signs while a major coronary artery is completely blocked. The heart can temporarily compensate for the damage, masking the internal crisis.
Does your pulse always race during a heart crisis?
No, while a fast pulse from adrenaline is common, severe heart attacks can damage the electrical system. This electrical damage can cause the heart rate to drop to dangerously slow and irregular levels.
Should I take my blood pressure if I have chest pain?
You can take it once if the machine is nearby, but do not obsess over the numbers. If you have severe, radiating chest pain or shortness of breath, immediately call for emergency services regardless of the reading.
Does high blood pressure mean I am having a heart attack right now?
Not necessarily. Severe stress, a panic attack, extreme physical pain from another injury, or a forgotten daily medication can all cause massive spikes. However, severe symptoms combined with a spike require immediate professional evaluation.
Conclusion
Understanding your cardiovascular system during a crisis is crucial, but relying solely on a home blood pressure monitor can be dangerous. Your numbers might look completely normal even while your heart muscle is actively starving for oxygen.
Long-term cardiovascular health requires a comprehensive approach: managing stress, controlling hypertension, taking prescribed medications, and maintaining a healthy diet and exercise routine. Never assume normal vitals grant you immunity from a cardiac event.
In the emergency room, physicians do not just look at blood pressure. They rely on electrocardiograms (ECGs) to track electrical activity, specific blood tests for cardiac proteins, and a thorough review of your symptoms and history to see the full clinical picture.
If you ever experience warning signs like severe chest pressure, sudden shortness of breath, or unexplained jaw pain, do not waste precious time checking your vitals at home.
When the heart is deprived of oxygen, every single minute dictates your survival. Put down the monitor and immediately call emergency medical services. Swift action and knowing these broader symptoms are your most powerful tools for saving your life.
Evidence-Based References:
- Mayo Clinic – Heart Attack (Symptoms & causes)
- Cleveland Clinic – Hypertension (High Blood Pressure): Symptoms and Causes
- National Heart, Lung, and Blood Institute (NHLBI)—What Is a Heart Attack
- American Heart Association (AHA) – Warning Signs of a Heart Attack
- Mayo Clinic – Hypertensive crisis: What are the symptoms?









