Can a Deviated Septum Cause Sleep Apnea? Symptoms & Treatments
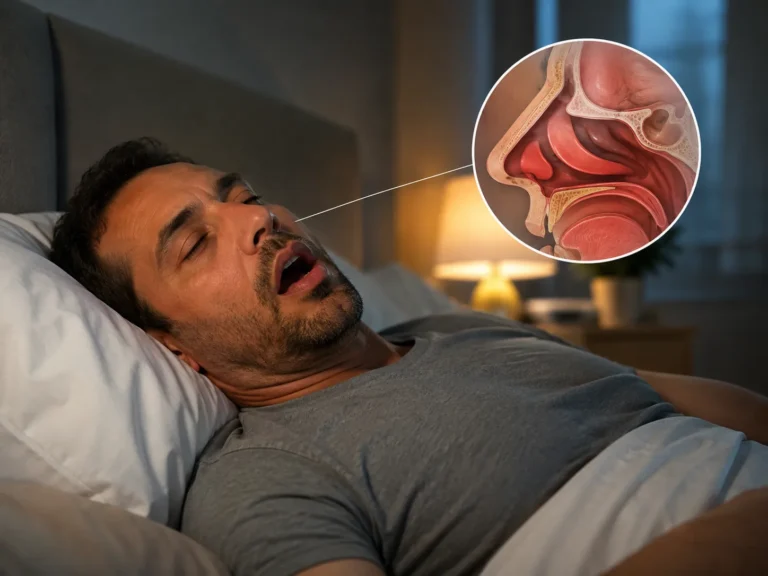
When patients arrive at the clinic exhausted and frustrated by poor rest, they often ask, can a deviated septum cause sleep apnea? It is a highly common and incredibly valid question. Many individuals suffer from chronic nasal congestion and assume their structural nose issues are the sole reason they stop breathing at night.
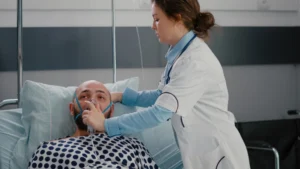
Understanding what sleep apnea is helps clarify this connection. In clinical practice, Dr. Julian Thorne frequently interviews patients who are confused between simple snoring and actual sleep apnea. Recently, Dr. Thorne evaluated a patient named Mark, who had a severely bent septum from a childhood sports injury.
Mark was convinced his nose was the entire reason for his extreme daytime fatigue and loud snoring. The American Academy of Sleep Medicine confirms these diagnostic challenges. During the consultation, Dr. Thorne had to clarify a crucial medical reality: not all nasal obstruction equals sleep apnea.
While a structural nose issue makes breathing difficult, sleep apnea typically involves the collapse of the airway deeper in the throat. This introduces a key conflict in sleep medicine.
We must differentiate between a structural nasal issue and true upper airway collapse. Understanding this distinction is vital for getting the right treatment, finding real relief, and finally achieving a restful night of sleep. Learn more about how REM sleep affects breathing patterns.
What Is a Deviated Septum?
Before connecting the conditions, we must understand the anatomy. The nasal septum is the wall of bone and cartilage that divides your nasal cavity into two distinct halves. Ideally, this septum is perfectly straight, allowing equal airflow through both nostrils.
However, when you have a deviated septum, this dividing wall is shifted or bent to one side. This displacement makes one nasal passage significantly smaller than the other. The Cleveland Clinic details nasal anatomy basics.
When patients ask, is a deviated septum bad?, the answer depends entirely on the severity of the deviation. Mild deviations are incredibly common and often go completely unnoticed. However, a severe deviation can severely impact airflow, leading patients to wonder, is a deviated septum dangerous?
While rarely life-threatening on its own, it drastically alters how air enters your respiratory system, forcing the body to work harder for every breath. Understanding when to seek professional evaluation helps with timely diagnosis.
Can a Deviated Septum Cause Sleep Apnea?
To answer directly, can a deviated septum cause sleep apnea? From a strict medical standpoint, there is an indirect relationship. A deviated septum alone does not typically cause obstructive sleep apnea (OSA), but it plays a massive role in its development and severity. The Centers for Disease Control and Prevention outlines OSA risk factors.
When you ask, “Does my deviated septum cause sleep apnea?” you must look at the chain reaction it creates. The structural bend creates high nasal resistance. Because breathing through the nose is difficult, your body instinctively switches to mouth breathing while you are unconscious. Mouth breathing is where the trouble begins.
When your mouth falls open during sleep, the jaw drops backward, pushing the tongue closer to the back of the throat. This significantly increases upper airway instability and creates the perfect environment for an airway collapse. The Mayo Clinic explains this physiological cascade.
Therefore, while answering can a deviated nasal septum cause obstructive sleep apnea, sleep specialists note that it is rarely the sole root cause. However, clinical sleep studies show that nasal obstruction significantly worsens existing OSA and leads to severe snoring and intense sleep fragmentation. Understanding how sleep quality affects health reinforces prevention urgency.
Can a Deviated Septum Cause Sleep Problems?

Even if it doesn’t cause full-blown apnea, can a deviated septum cause sleep problems? Absolutely. Nasal obstruction is a primary culprit for poor sleep architecture. When your nasal passages are blocked, you cannot efficiently filter, warm, or humidify the air you breathe.
This chronic mouth breathing leads to waking up with a severely dry mouth, a sore throat, and profound daytime fatigue. The Healthline reviews sleep disruption mechanisms.
Patients frequently ask, can deviated septum cause snoring? Yes, and it is often very loud. The restricted airflow creates turbulence, causing the tissues in the nose and throat to vibrate violently.
Therefore, deviated septum and snoring are heavily linked, even in patients who do not actually stop breathing during the night. For broader wellness strategies, see our guide on exercise benefits for sleep health.
Can a Deviated Septum Be Mistaken for Sleep Apnea?
Because the symptoms overlap so heavily, can a deviated septum be mistaken for sleep apnea? Yes, both by patients and sometimes by primary care providers without specialized sleep testing. Both conditions share highly similar daily struggles.
Common deviated septum symptoms include loud snoring, waking up unrefreshed, chronic fatigue, and generally poor sleep quality. A patient observing these issues might immediately assume they have OSA. The
details symptom differentiation.
The key medical difference lies in what happens to the breath. In sleep apnea, breathing literally stops for 10 seconds or more due to a throat collapse.
With a deviated septum, the airflow is heavily restricted and noisy, but the actual breathing effort and flow (even if through the mouth) rarely stop completely. Understanding cardiovascular symptoms linked to sleep disorders helps with accurate diagnosis.
Symptoms of Deviated Septum That Affect Sleep
If you suspect your nose is ruining your rest, you must look for specific clinical signs. Deviated septum symptoms extend far beyond just feeling “stuffy.” A primary indicator is persistent, one-sided nasal blockage.
You may notice that you can only comfortably breathe through one nostril, especially when lying down. This physical blockage forces positional sleeping that can cause major discomfort. The Medical News Today reviews nasal obstruction symptoms.
Additionally, patients frequently suffer from breathing problems that trigger intense sinus pressure. This lack of proper sinus drainage leads to chronic morning headaches. Combined with loud snoring and chronic mouth breathing, these sleep disturbance patterns ruin your sleep cycles. For context on how sleep issues mimic ADHD symptoms, see our mental health resource.
Does a Deviated Septum Worsen Obstructive Sleep Apnea (OSA)?
For patients already diagnosed with sleep apnea, the situation becomes more complex. Does deviated septum worsen osa? Yes, exponentially. The pathophysiology of OSA involves the collapse of the soft tissues in the throat.
When you have high nasal resistance from a bent septum, your lungs have to pull much harder to draw air in. This creates high “negative airway pressure” in the throat. The National Heart, Lung, and Blood Institute explains OSA mechanics.
This intense suction effect acts like a vacuum, forcefully pulling the relaxed throat tissues inward and causing them to collapse faster and more frequently.
Furthermore, this structural issue dramatically increases the risk of CPAP intolerance, making the primary treatment for OSA incredibly difficult to endure. Understanding how sleep duration affects health reinforces treatment importance.
Using CPAP With a Deviated Septum
Treating sleep apnea usually involves continuous positive airway pressure. However, using cpap with deviated septum presents a unique set of frustrating challenges. When one nasal passage is blocked, forcing high-pressure air through the nose can cause intense nasal CPAP discomfort, burning, and severe dryness.
Patients often instinctively open their mouths, leading to massive mask leakage issues and therapy failure. The National Sleep Foundation offers CPAP management tips.
To combat this, sleep specialists often recommend specialized heated humidification solutions to soothe the nasal passages.
Furthermore, switching from a simple nasal mask to a full-face mask is often required, allowing the CPAP pressure to enter through both the nose and the mouth to bypass the septal blockage. For comprehensive wellness strategies, explore our guide on how to maintain a healthy lifestyle.
Treatment Options for Deviated Septum and Sleep Apnea
When managing both conditions, a comprehensive medical approach is required. Deviated septum sleep apnea treatment is not a one-size-fits-all scenario. To truly answer, can a deviated nasal septum be fixed?
We must explore the full spectrum of care, starting from conservative management to surgical intervention. This multifaceted approach is what Dr. Thorne utilizes to ensure patients achieve long-term relief rather than temporary fixes. The Johns Hopkins Medicine details treatment protocols.
Non-Surgical Medical Management
For many patients, the goal is to optimize the airway without going under the knife. Non-surgical treatments focus on reducing any additional inflammation inside the nose that might be making the deviation worse. Doctors frequently prescribe prescription nasal corticosteroids.
These powerful anti-inflammatory sprays reduce the swelling of the nasal lining, creating slightly more room for air to pass around the deviated bone. Additionally, daily saline irrigations and targeted antihistamines are used to clear out allergens and mucus.
While these medications cannot straighten the bone or cartilage, they often reduce the total nasal airflow restriction enough to make breathing comfortably possible. The Britannica explains nasal anatomy and treatment basics.
Advanced CPAP Management
If the patient has confirmed OSA, managing the CPAP machine alongside the structural nasal issue is the next critical step. This requires precise clinical adjustments by a sleep technician. Because the nasal resistance is high, standard CPAP pressures might feel suffocating.
Doctors often utilize Auto-CPAP (APAP) machines that dynamically adjust the pressure, delivering only what is needed at any given moment. Mask selection is arguably the most important factor here. As mentioned, full-face masks are often the gold standard for these patients.
By covering both the nose and mouth, the machine ensures that even if the nasal passage is entirely blocked by the septum, the therapeutic air pressure still successfully reaches the airway to prevent collapse.
Surgical Interventions: The Septoplasty
When non-surgical methods fail and the patient’s quality of life is severely impacted, surgery becomes the most viable option. The specific procedure to correct this is called a septoplasty. During a septoplasty, an ear, nose, and throat (ENT) surgeon works entirely inside the nose.
They lift the mucous membrane, reshape, reposition, or remove the bent portions of the cartilage and bone, and then lay the membrane back down. The recovery timeline generally involves a few days of swelling, congestion, and mild discomfort, with most patients returning to normal activities within a week.
The expected outcomes are usually excellent for restoring nasal airflow, drastically reducing snoring, and making CPAP therapy incredibly comfortable and effective again. Often, surgeons will simultaneously perform a turbinate reduction to maximize the newly opened airway. The American Academy of Otolaryngology provides surgical guidance.
Is Surgery for a Deviated Septum Worth It?

Patients facing the prospect of an operation naturally ask, is surgery for a deviated septum worth it? The answer depends on your primary medical goal. If your goal is to breathe clearly through your nose, eliminate chronic sinus infections, and stop violent snoring, the surgery has a very high success rate.
It drastically improves overall sleep quality. However, realistic expectations are crucial. It is important to know when it does NOT cure sleep apnea. If you have severe obesity or a naturally narrow throat, fixing the nose will not stop your throat from collapsing.
In clinical ENT practice, patients sometimes report persistent fatigue after nasal surgery, highlighting that the nose is only one component of the airway. For weight management support, see our guide on healthy diet principles.
Can Fixing a Deviated Septum Stop Sleep Apnea?
This leads to the ultimate question: will fixing a deviated septum stop sleep apnea, or can a deviated septum cure sleep apnea entirely? The clear clinical answer is that it dramatically improves symptoms, but it rarely cures OSA alone.
Straightening the septum removes the vacuum effect and stops the mouth-breathing trigger, which can lower your Apnea-Hypopnea Index (AHI) score. However, true resolution usually requires a combination treatment approach.
Correcting the septum makes the airway healthier, but patients often still need mild CPAP therapy, weight management, or a custom oral appliance to ensure the throat remains fully open during deep sleep. The Harvard Health Publishing reviews combination therapy efficacy.
Deviated Septum and Sleep Apnea VA Disability
For military veterans, the link between these conditions has major legal and financial implications. Navigating deviated septum and sleep apnea VA disability claims requires understanding specific medical rules. The VA typically views sleep apnea as a separate condition.
However, through a concept called “secondary service connection,” veterans can argue that a service-connected nasal injury (like a broken nose causing a deviated septum) directly worsened or caused their OSA. Winning this claim requires meticulous medical documentation.
Veterans must provide concrete ENT records showing the structural damage, alongside a formal sleep study proving the apnea, and a “nexus letter” from a doctor linking the two conditions together. The U.S. Department of Veterans Affairs provides disability claim guidance.
Frequently Asked Questions
Can a deviated septum cause obstructive sleep apnea?
Indirectly, yes. While it does not cause the throat collapse itself, the severe nasal blockage forces mouth breathing and increases airway resistance, which can trigger or significantly worsen existing obstructive sleep apnea. The World Health Organization confirms global sleep disorder risk factors.
Can a deviated septum cause snoring?
Yes, it is a leading cause of severe snoring. The restricted nasal passage creates highly turbulent airflow, causing the tissues in the nose, soft palate, and throat to vibrate loudly as air is forced past the blockage. Understanding healthy sleep practices helps reduce snoring triggers.
Can a deviated septum cause breathing problems?
Absolutely. A severe deviation physically blocks air from entering one or both nostrils, leading to chronic congestion, the inability to breathe through the nose during exercise, and heavy reliance on mouth breathing. The American Heart Association details cardiovascular impacts of breathing disorders.
Can a deviated septum cause headaches?
Yes. When the septum blocks the normal drainage pathways of the sinus cavities, pressure builds up rapidly. This trapped pressure often results in chronic, throbbing headaches, particularly around the eyes and forehead in the mornings. For headache management tips, see our guide on how to deal with stress.
Can a deviated nasal septum be fixed?
Yes, it can be permanently fixed through a routine surgical procedure known as a septoplasty. An ENT surgeon straightens the cartilage and bone inside the nose, permanently opening the nasal passages and restoring normal airflow. The National Institute of Neurological Disorders and Stroke provides neurological context for sleep-related interventions.
Conclusion
Understanding the complex relationship between your nasal structure and your sleep quality is the first step toward better health. While a deviated septum may not be the sole cause of sleep apnea, it is an undeniable instigator that worsens snoring, fuels daytime exhaustion, and complicates treatment.
Do not dismiss chronic nasal blockage as just a minor annoyance. If you are struggling with severe snoring and waking up exhausted, consulting with an ENT or a sleep medicine specialist is crucial.
By addressing both the structural nasal issues and the deeper airway mechanics, you can finally reclaim the restful, restorative sleep your body desperately needs. For comprehensive cardiovascular prevention strategies, explore our guide on how to prevent heart disease.
Authoritative References
- World Health Organization. (2026). Healthy sleep and neurological health fact sheet. https://www.who.int/news-room/fact-sheets/detail/sleep-and-health
- WebMD. (2025). Sleep apnea headaches: Causes and relief strategies. https://www.webmd.com/sleep-disorders/sleep-apnea/sleep-apnea-headaches
- Medical News Today. (2026). How sleep apnea affects brain health and headache risk. https://www.medicalnewstoday.com/articles/sleep-apnea-headaches
- Johns Hopkins Medicine. (2025). Sleep apnea: Diagnosis and treatment overview. https://www.hopkinsmedicine.org/health/conditions-and-diseases/sleep-apnea
- Britannica. (2026). Sleep disorders and neurological impacts. https://www.britannica.com/science/sleep-disorder
- American Heart Association. (2025). Sleep apnea and cardiovascular risk connection. https://www.heart.org/en/health-topics/sleep-disorders/sleep-apnea-and-heart-disease
- Healthline. (2026). Morning headaches: Causes linked to sleep quality. https://www.healthline.com/health/morning-headaches-sleep-apnea
- National Institute of Neurological Disorders and Stroke. (2025). Headache information page. https://www.ninds.nih.gov/health-information/disorders/headache
- Sleep Education (AASM). (2026). Sleep apnea symptoms and treatment options. https://sleepeducation.org/sleep-disorders/sleep-apnea/
- Harvard T.H. Chan School of Public Health. (2025). Sleep and chronic disease prevention. https://www.hsph.harvard.edu/nutritionsource/sleep/